Atrial Fibrillation (also called AF or A Fib) is a common heart rhythm disorder caused by a problem in the conduction of electrical impulses in the upper chambers, or atria, of the heart. A Fib and other rapid heartbeats that arise in the atria, or in the juncture between the atria and the lower chambers (ventricles) are called "supraventricular tachycardias."
 |
|
More than 2 million people in the U.S. have A Fib, and about 160,000 new cases are diagnosed each year. A Fib is uncommon among young people, although it can occur in people of any age. The likelihood of developing the condition, however, increases as we get older. After age 65, between 3 percent and 5 percent of people have atrial fibrillation. Approximately 9 percent of people who are age 80 or older have the condition.
|
What Causes A Fib? |
|
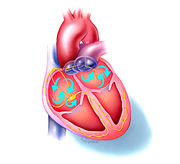
In A Fib, the electrical signals that coordinate the muscle of the upper chambers (atria) of the heart become rapid and disorganized, typically causing the atria to beat faster than 300 beats per minute. (The normal rate when the heart is at rest is about 60 to 80 beats per minute). When this happens, the atria may contract poorly and no longer effectively force blood into the lower chambers (ventricles). As a result, the flow of blood to the body may be reduced. Atrial fibrillation may occur from time-to-time, or it may be a permanent condition.
 |
|
|
|
|
|
Types of Atrial Fibrillation
|
|||
|
|
Health RisksIn younger people who have no other disease that affects the heart, atrial fibrillation or flutter usually is not considered serious. Some people with atrial fibrillation, however, are at increased risk of stroke, heart failure or heart muscle disease. Sometimes, A Fib can damage heart muscle and alter the normal electrical signals to the heart. This may change the patterns of contraction and relaxation of heart muscle. This is known as electrical remodeling.
|
|
|
|
An Increased Risk of Stroke
|
|
|
|||
Atrial Flutter |
|||
| Atrial flutter (AFL) is very similar to atrial fibrillation. Both conditions are types of supraventricular (above the ventricles) tachycardia (rapid heart beat). This means that the upper chambers (atria) of the heart beat too fast. This produces muscle contractions that are out of sync with the lower chambers (ventricles). Sometimes, the muscle of the atria contracts, or beats, as many as 250 to 400 beats per minute. Usually the individual's pulse may be less rapid. This is because the heart has a built-in "gate" (the atrioventricular (AV) node) that controls the number of electrical impulses that travel from the atria to the ventricles. | |||
|
|||
| Symptoms | |||
| The signal that causes AFL circulates in an organized, predictable pattern, so people with atrial flutter usually continue to have a steady heartbeat, even though it is faster than normal. (In Atrial fibrillation, on the other hand, the electrical signals are chaotic causing the atria to spasm and quiver. People with A Fib may feel that the heart is skipping beats, or the pulse is "out of rhythm"). In AFL, the too-rapid heartbeat sometimes is described as a "flutter," or tremor-like movement of the heart. Some patients have no other symptoms, but others feel shortness of breath, fatigue, dizziness or even fainting (syncope - click for more info). AFL is likely to last for days or weeks at a time. Most people with AFL require treatment to interrupt the abnormal circuit and slow the heartbeat to its normal rate. With proper treatment, AFL is rarely life-threatening. But, like atrial fibrillation, AFL may increase a person's chance of having a stroke. This is because when the atrial muscle is not contracting properly, it cannot pump a normal amount of blood into the ventricle. Some of the blood is left behind and may form pools. Pooled blood that is not in circulation is more likely to form clots. A blood clot can break off and travel to the vessels in the brain. If a clot blocks the blood supply to the brain, the result is stroke. If the heart beats rapidly for a long time, the muscle of the ventricle may weaken and lose some of its ability to pump blood to other parts of the body. This can increase the risk of more serious heart disorders such as heart failure. | |||
| The Role of the Heart's Natural Conduction System | |||
| The pumping of the heart is controlled by steady electrical signals produced by the heart's natural pacemaker, the sinoatrial (SA) node, located in the right atrium. The SA node passes signals through the atria to the atrioventricular (AV) node. The AV node is the electrical "gate" or "junction box" that receives the signals and passes them along to the ventricles. When the AV node receives signals that are too rapid, such as in atrial flutter (and A Fib) its job is to slow them down so that there will be enough time for the blood in the atria to enter the ventricles. The signals passed from the AV node travel along fibers called bundle branches, causing the ventricles to contract and pump blood out to the body. The heart normally rests until the next signal from the SA node begins the cycle again. (For more information on the heart's conduction system, visit the normal heart). | |||
| In AFL, the AV node compensates for the abnormal signals coming from the atria by blocking some of them, so that only a fraction (typically one-half to one-fourth) reaches the ventricles. Even though the electrical signals from the atria may be as rapid as 300 or more beats per minute, a person with AFL may have a lower pulse rate (from 75 to 150 beats per minute). Nonetheless, the pulse rate often is abnormally high (a normal pulse for an individual at rest is about 60 to 80 beats per minute) and most patients will experience some symptoms. |




